Thank you to all the PAs who took the time to complete our survey on the impact of the Leng Review. Your voices have provided crucial evidence that we will use to strengthen our judicial review and advocacy work.
Between December and January, we asked you to share your experiences of how the Leng Review has impacted your scope of practice, your departments, and most importantly, patient care. Your responses represent a significant cross-section of our profession – from general practice to urgent and emergency care, and across all regions. The results paint a stark picture of the detrimental impact these recommendations have had on PAs, patients, and the wider NHS workforce.
The Results
“It’s been horrendous and an absolute disaster for the profession,” said a PA working in Primary Care in Lancashire.
76% of PAs have had their scope of practice restricted since the Leng Review was published in July. Far from being only about professional satisfaction, this has a direct impact on patients.
PAs are seeing fewer patients. The data shows a dramatic shift in how PAs are being deployed. Before the Leng Review, many PAs were averaging 11+ patient interactions (including consultations, follow ups, results, referrals, etc) per shift. Since July, those numbers have plummeted, while the number of PAs seeing only 1-5 patients per shift has more than quadrupled (see figure 1).
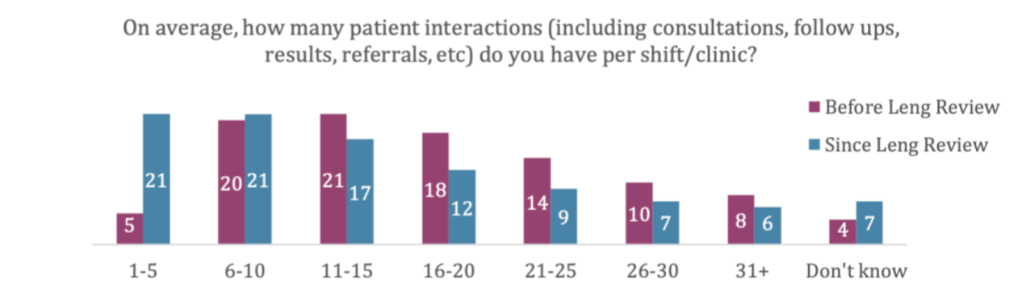
This represents a massive underutilisation of qualified medical professionals at a time when the NHS is facing unprecedented demand. PAs with the competencies to manage substantial patient caseloads are now sitting idle or restricted to administrative tasks while patients wait longer for care.
Patient waiting times are getting worse. Two in five PAs reported worsening waiting times in their departments since the Leng Review:
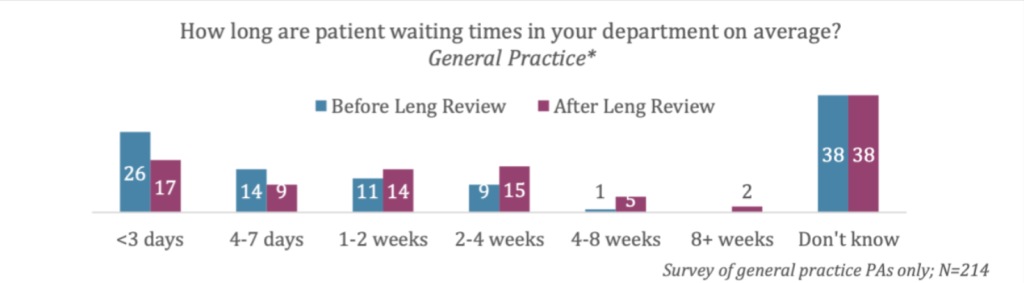
In urgent and emergency care, the PAs we surveyed reported that patient waiting times increased following the Leng Review. In general practice, PAs reporting average waiting times of under a week has dropped from 40% to 26% (see figure 2).
One PA working in secondary care in Cheshire described a patient with sepsis who had to wait more than three hours for clinical review and antibiotics because no doctor was available, even though the PA was free to help. “Pre-Leng I could have reviewed patient, discussed with senior and commenced on sepsis pathway,” they explained. “The longer the wait for antibiotics, the higher the mortality rate.”
The survey shows a clear shift away from rapid access to care, with waiting times lengthening across the board. When you consider that PAs undertake approximately 20 million appointments annually, even small delays per patient compound into massive backlogs across the system.
The Impact on Doctors and Supervisors
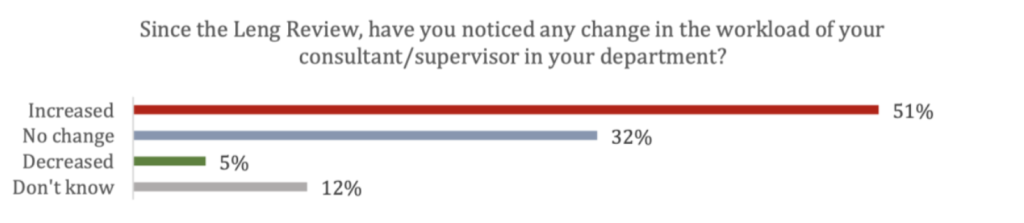
This isn’t just affecting PAs and patients. Over half of you (51%) report that your consultant or supervisor’s workload has increased as a result of the Leng Review. Doctors are now doing work that PAs were trained, qualified, and competent to do – work they were doing safely and effectively before July (see figure 3).
A PA in Lancashire captured the frustration many are feeling: “The increased supervision is taking doctors away from other work, although every doctor I work with agrees the increased supervision is not necessary as I’m trusted (the supervision agreed before the Leng review was absolutely adequate) – it’s a box ticking exercise from the Leng Review. It just takes up time.”
This defeats one of the core purposes of the PA role: to work alongside doctors to improve access to care and reduce clinical workload. Instead of supporting the medical workforce, the Leng Review has added to the burden doctors are already carrying.
The Wider Impact
Beyond the statistics, your responses revealed the multiple ways these changes are causing harm across the NHS.
Continuity of care is being destroyed. A PA in Staffordshire who had been building relationships with mental health patients for three years explained: “I’ve been getting to know my current patients for three years, and now they are having to see people who they have never met before. My regular mental health follow-ups have been put on the doctors.” These established therapeutic relationships – built over years of consistent care – are being abandoned overnight.
Administrative systems are in chaos. Multiple PAs described reception teams confused about booking protocols, causing delays and frustration for patients and staff alike. As a PA in London put it: “Reception team are unsure of patients they should/shouldn’t book with me leading to potential delays. It is offering a lesser service to patients who should always be the priority in the NHS.”
The emotional toll on PAs is severe. A PA in Lancashire captured what many of you are feeling: “The total loss of autonomy is demoralising, has taken away all job satisfaction, and reduced confidence as you feel like a student again. It’s been horrendous and an absolute disaster for the profession.”
These aren’t isolated incidents. They represent a pattern of harm caused by implementing sweeping recommendations without proper assessment of their real-world impact.
What this means:
Commenting on the results, UMAPs General Secretary Stephen Nash says:
“The terrible impact of the Leng Review recommendations should have been entirely obvious to both the government and NHS England. Effectively sidelining some 3,500 highly qualified medical professionals was clearly going to be disastrous for patients, associates, and doctors alike. Yet at no point did the Health Secretary make any assessment of how this would harm medical associates or restrict patients’ access to care.
Far from protecting patients, it is increasingly looking like these changes were cooked up to mollify the increasingly radical BMA, which at the time of the review was threatening major strike action. That is why we are challenging the irrational recommendations in our judicial review, ensuring that PAs and AAs can go back to caring for patients and helping our doctor colleagues to shoulder the burden.”
What Happens Next
This evidence strengthens our judicial review case against the Health Secretary, NHS England, and Professor Leng, demonstrating that these recommendations were implemented without any proper assessment of their impact on patient care or the NHS workforce.
We expect our permission to proceed hearing this spring, with the full case likely to be heard later this year. Your responses will help our legal team, led by Patrick Green KC, build the strongest possible case.
Beyond the judicial review, we’ll be using this evidence in our ongoing advocacy work with NHS England, policymakers, and the media to ensure the real-world impact of the Leng Review cannot be ignored or dismissed.
Thank You
Your dedication to completing this survey during the busy festive period shows the commitment you have to our profession and to patient care. You’ve given us powerful evidence that these changes are harming patients, overloading doctors, and wasting the skills of 3,500 highly qualified medical professionals.
We will continue to fight for your right to practice to the full extent of your training and experience. Together, we’re protecting our profession – and the patients who rely on us.
If you’re facing scope restrictions, workplace issues, or need support, please don’t hesitate to contact us here: Help Request Form
Notes to Methodology
- UMAPs surveyed 459 PAs currently working clinically across NHS England.
- The sample includes a spread across NHS England regions and departments, with 47% of respondents working in general practice and 27% in urgent and emergency care. Over half have been working as a PA for more than five years.
- Fieldwork was conducted between 17 December 2025 and 14 January 2026. The survey was fielded online and open to all PAs working clinically.







